According to the American Cancer Society, prostate cancer is the second most common cancer in American men, averaging around 175,000 new cases every year. During the diagnosis process, more than one million men in the U.S. alone undergo a prostate biopsy, a procedure that results in 10-12 needle cores for patients, and more than 10 million tissue samples that need to be examined by pathologists.
To help alleviate the strain on uropathologists, reduce workloads, and harmonize grading, a team of researchers from 26 worldwide organizations developed a deep learning-based solution to detect and grade cancer in prostate needle biopsy samples.
“AI has potential to reduce high intra-observer variability and to provide diagnostic expertise in regions where this is currently unavailable,” the researchers stated in their paper. “It is recognized that there is a shortage of pathologists internationally. In China, there is only one pathologist per 130,000 population, while in many African countries the ratio is of the order of one per million.”
Using two NVIDIA GPU clusters, comprised of NVIDIA Tesla P100 GPUs, distributed among 27 nodes at the Tampere Center for Scientific Computing in Finland, running CUDA, cuDNN, MATLAB, Keras, TensorFlow and XGBoost, the team trained two deep neural networks for classification of image patches and multiple convolutional neural networks on a selection of 6,682 biopsies from 976 men.
The cases selected for this study were chosen to represent the full range of diagnoses, the researchers said.
In addition to the training set, the team also used 1,630 biopsies from 245 men to evaluate the performance of the deep learning system.
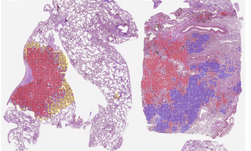
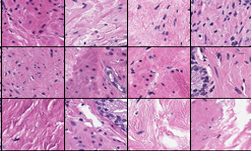
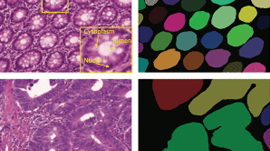
Overview of the artificial intelligence system. The tissue region in the input WSI is split into patches (top). The patches are fed as input to a detection ensemble of 30 DNNs for discriminating between benign and malignant patches (left box; top row), and to a grading ensemble of 30 DNNs for classifying patches into Gleason grades 3, 4 and 5 (right box; top row). In the patchlevel prediction phase (both boxes; middle row), each trained DNN outputs a vector of class-wise probabilities for each input patch. The class-wise probabilities, indicated here with squares where the grayscale intensity corresponds to probability value, are mapped back to the locations of the corresponding patches in the WSI to construct a probability map for each class. The maps are summarized into features, which are used as inputs to train ensembles of boosted trees to predict cancer presence and extent (left box; bottom row) and grade (right box; bottom row) for entire WSIs. In the WSI-level prediction phase, outputs from the 30 boosted trees in each ensemble are averaged, and the final classification of each WSI is assigned to the class associated with the highest average probability.
The algorithm achieved accuracy in the range of 0.997 and 0.999, on par with a human pathologist who achieved an accuracy level of 0.96.
“Here, we have for the first time demonstrated AI-based grading of prostate biopsies on the level of leading urological pathologists,” the researchers said. “We believe that the use of this system can increase sensitivity and promote patient safety by providing decision-support and by focusing the attention of the pathologist on regions of interest.”
The study was recently published on ArXiv. The team has also made available an online demo that allows users to visually examine predictions generated for 30 biopsies.